The HIS market in 2026: What the data shows
Understanding the market context helps put individual vendor claims in perspective.
The global hospital information system market is valued at USD 61.46 billion in 2025 and is forecast to reach USD 86.01 billion by 2030, growing at a CAGR of 6.95%. Cloud-based deployment is the fastest-growing segment, at 10.69% CAGR, reflecting a broad industry shift away from on-premise infrastructure.
Market concentration is high. In the US acute care hospital segment, three vendors dominate: Epic holds 42.3% market share, Oracle Health 22.9%, and MEDITECH 14.8%. In 2024, Epic added a net 176 hospitals, its largest annual gain on record, while Oracle lost 74 and MEDITECH declined by 57.
But US acute care is only one segment of the market. Mid-size hospitals, rural facilities, specialty centers, and hospitals in Asia-Pacific and EMEA operate with very different needs, budgets, and regulatory environments. Those segments are where the more diverse vendor landscape lives.
One more trend worth noting: the EHR/EMR system segment accounts for the largest share of HIS software spend, but hospitals increasingly evaluate vendors on broader criteria, including interoperability standards (HL7 FHIR), AI-assisted documentation, population health tools, and total cost of ownership over 10 years, not just licensing fees.
How to use this guide: Match by hospital type
Before looking at any vendor, answer these two questions:
What is your facility size and type?
- Large health systems and academic medical centers (500+ beds, multi-site)
- Mid-size hospitals (100-500 beds, community or regional)
- Small hospitals, rural facilities, and clinics (under 100 beds)
- Facilities needing a custom-built system
What is your primary constraint?
- Budget (OTS SaaS vs. enterprise licensing vs. custom build)
- Compliance (HIPAA, GDPR, local DOH/MOH requirements, HL7/FHIR standards)
- Interoperability (connecting to existing lab, imaging, or billing systems)
- Flexibility (how much the system needs to match your workflows vs. adapting your workflows to the system)
The sections below are organized by hospital type. Each includes the top 2-3 options, their strengths, their real limitations, and who they are best for.
Before comparing systems, see what benefits and limitations to expect from any HIS to sharpen your evaluation criteria.
Best HIS for large hospitals and health systems
Large health systems need enterprise-grade scalability, deep interoperability, and AI-assisted clinical tools. The short list is dominated by two players.
1. Epic Systems

Epic is the market leader by a wide margin. It holds 42.3% of the US acute care hospital market and serves 305 million patient records globally through its MyChart portal, with installations in over 3,700 hospitals and 45,000 clinics.
What makes it the default choice for large health systems is not just its feature set, but its ecosystem: a large network of third-party developers, deep HL7 FHIR interoperability, and a track record of successful deployments at the most complex healthcare organizations in the world, including Mayo Clinic, Johns Hopkins, Cleveland Clinic, and Kaiser Permanente.
In 2024, Epic adopted USCDI v3 federal data exchange standards ahead of the December 2025 deadline, reinforcing its position as the interoperability benchmark for the industry.
Strengths: Unmatched feature depth, best-in-class interoperability, AI-assisted documentation, strong patient engagement tools (MyChart), and the most robust third-party app marketplace in the industry.
Real limitations: Implementation costs are substantial, with estimates around $16 million for a mid-sized hospital and timelines of 12-24 months – see the hospital information system cost guide for a full breakdown. Epic has faced criticism in several international rollouts, including significant issues in Norway where over 90% of affected doctors considered the system a threat to patient health within the first year of implementation. It is also expensive for smaller organizations and generally not worth evaluating unless you have both the budget and the IT infrastructure to support it.
Best for: Large hospital networks, academic medical centers, and integrated delivery networks in North America and selected international markets.
2. Oracle Health (formerly Cerner)
Oracle Health holds 22.9% of the US acute care market and became the second-largest HIS vendor after Oracle acquired Cerner for $28.3 billion in 2022. It serves large health systems, government hospitals, and the US Department of Veterans Affairs.
In 2025, Oracle launched a next-generation EHR built on Oracle Cloud Infrastructure (OCI) with an embedded AI voice interface called “Clinical AI Agent“, designed to reduce physician documentation time through ambient listening and automated clinical notes. Early reports show documentation time reductions and positive momentum after several rocky years following the Cerner acquisition.
Oracle’s cloud-native approach offers faster deployment and lower total cost of ownership compared to Epic for many organizations, particularly those that already operate on Oracle infrastructure. However, healthcare organizations have cited poor partnership and inconsistent follow-through as ongoing concerns, and Oracle saw a net loss of 74 hospitals in 2024.
Strengths: Cloud-native architecture, strong enterprise security and compliance credentials (especially for global deployments), AI-powered documentation tools, and a lower TCO trajectory than Epic for cloud-first organizations.
Real limitations: A difficult few years post-acquisition have damaged trust. Oracle declined to share its new contract list with KLAS in 2024, an unusual move that signals ongoing challenges. Implementations have been inconsistent.
Best for: Large health systems already in the Oracle ecosystem, government and VA-affiliated hospitals, and organizations prioritizing cloud-native infrastructure and AI-first workflows.
Best HIS for mid-size hospitals
The 100-500 bed segment is where the market is most competitive. These hospitals need a full-featured HIS but cannot absorb the cost and complexity of an Epic implementation. Three options stand out.
3. MEDITECH Expanse
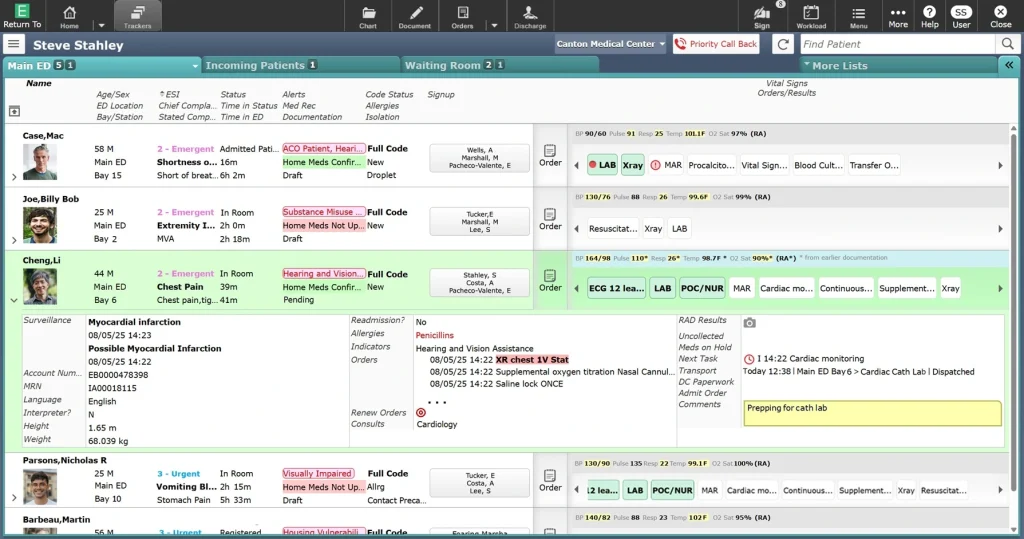
MEDITECH holds 14.8% of the US acute care market and has consistently ranked in the top two for mid-size hospitals (151-400 beds) in KLAS evaluations for five consecutive years. In 2025 alone, 15 rural hospitals selected MEDITECH Expanse via its MaaS (MEDITECH-as-a-Service) cloud platform, drawn by its ability to deliver enterprise-grade features without requiring large IT teams or capital infrastructure.
Expanse is a fully web-based EHR with strong interoperability through its Traverse Exchange network, AI-assisted documentation tools including ambient listening and auto-generated discharge summaries, and solid patient engagement features. HCA Healthcare, one of the largest US hospital operators, has deployed Expanse across 182 hospitals.
User reviews highlight ease of navigation and a manageable implementation process, though some flag limited customization options and analytics tools that feel basic compared to Epic.
Strengths: Proven in the mid-size segment, strong KLAS ratings, cloud-native MaaS model reduces infrastructure burden, good value for money relative to Epic and Oracle.
Real limitations: Limited customization for complex or highly specialized needs. Third-party integrations are not always seamless. Reporting and analytics tools are solid but not best-in-class. No public API available.
Best for: Community hospitals, regional health systems, and rural hospitals in the 100-500 bed range looking for a proven, cost-effective system with enterprise-grade features and minimal IT overhead.
4. Insta HMS
Insta HMS is a comprehensive hospital management system with a strong presence in South and Southeast Asia, the Middle East, and Africa. It covers a wide module set including OPD, IPD, emergency, operating theater, pharmacy, lab, radiology, billing, and HR management, and supports both cloud and on-premise deployment.
It is one of the more affordable full-featured options for international markets where Epic and Oracle are either priced out of reach or poorly localized. User reviews on platforms like Capterra and G2 generally rate the system positively for feature breadth, though some flag occasional performance issues and a learning curve for staff.
Strengths: Wide module coverage, affordable relative to US enterprise vendors, strong regional support in Asia, Middle East, and Africa, multi-language support.
Best for: Mid-size hospitals in Asia-Pacific, MENA, and Africa looking for a cost-effective full-suite HIS with regional support.
5. eClinicalWorks
eClinicalWorks is a US-based EHR and practice management platform with over 180,000 healthcare professionals using it across ambulatory and hospital settings. It is cloud-based, covers telehealth, population health, revenue cycle management, and AI-assisted documentation, and is competitively priced for the mid-market.
It is more commonly deployed in ambulatory and outpatient settings than inpatient hospitals, but its broad feature set and telehealth integration make it a practical option for multi-specialty clinics and outpatient-heavy facilities.
Strengths: Competitive pricing, strong telehealth integration, large US user base, broad ambulatory feature set.
Real limitations: Better suited for outpatient than inpatient care. Has faced regulatory scrutiny in the past over data accuracy issues, which potential buyers should research before committing.
Best for: Multi-specialty clinics, outpatient facilities, and telehealth-forward organizations in the US market.
Best HIS for small hospitals, clinics, and rural facilities
Smaller facilities need systems that are fast to deploy, affordable, and do not require large IT teams to maintain. The priorities shift toward ease of use, cloud hosting, and essential modules rather than enterprise-scale feature depth.
6. Aarogya
Aarogya is a hospital information management system designed for small-to-large hospitals, with a focus on streamlining daily operations through a comprehensive ERP-style approach. It covers administrative, clinical, and financial functions in a single platform and is well-regarded for its user-friendly interface and complete application cycle coverage.
Strengths: Comprehensive module set, user-friendly, suited for facilities that want a single system covering everything from pharmacy to HR.
Real limitations: Less established outside South Asia. Limited third-party integration ecosystem compared to enterprise vendors.
Best for: Small-to-mid size hospitals in South Asia and international markets looking for an affordable, full-coverage HIS without the overhead of enterprise vendors.
7. eVisit
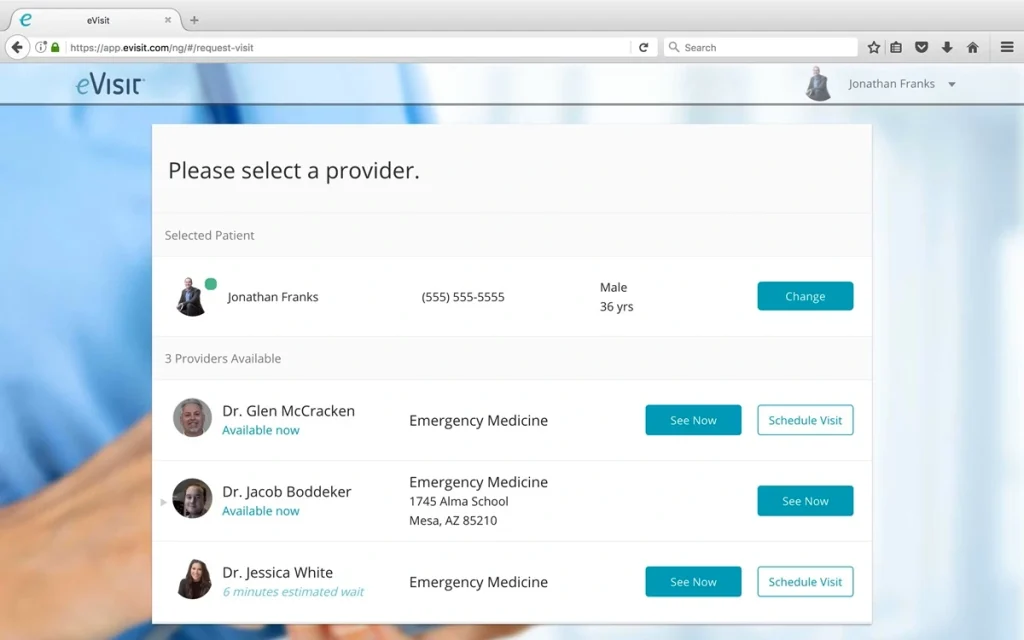
eVisit is a cloud-based platform focused on improving patient access and satisfaction. It covers medical charting, data collection, billing, reimbursement management, payment processing, and ePrescription. Its standout feature is patient self-service: online scheduling, real-time charting, and telehealth-first workflows that reduce administrative burden.
Users consistently highlight the ease of appointment scheduling and helpful customer support. The main drawbacks cited in reviews are occasional system glitches and higher-than-average pricing for smaller practices.
Strengths: Excellent patient engagement tools, strong telehealth integration, intuitive interface for both patients and staff.
Real limitations: Occasional system reliability issues flagged in user reviews. Pricing can be high for small independent practices.
Best for: Small-to-medium private practices, outpatient clinics, and telehealth-forward facilities where patient experience and ease of access are the primary differentiators.
8. OpenMRS
OpenMRS is an open-source medical record system originally developed by Partners in Health and the Regenstrief Institute, with a global community of implementers and contributors. It has been deployed in over 40 countries, with particularly strong adoption in sub-Saharan Africa, Southeast Asia, and other low-resource settings.
The system is modular and highly customizable, supporting HL7 and FHIR standards, and has been used to manage patient data for HIV programs, tuberculosis treatment, maternal health, and general hospital management in resource-constrained environments. Because it is open-source, there are no licensing fees, though implementation, hosting, and maintenance costs apply.
Strengths: Free and open-source, highly customizable, strong international community, proven in low-resource and NGO-funded healthcare settings, FHIR/HL7 compliant.
Real limitations: Requires technical expertise to implement and maintain. Not suited for facilities without access to development support. UI can be dated depending on the version and modules deployed.
Best for: Government hospitals, NGOs, and public health programs in low-to-middle income countries, as well as facilities with technical capacity to self-implement and maintain an open-source platform.
Best HIS for custom development
Off-the-shelf systems are built around common workflows. When your hospital’s workflows are genuinely complex, when you are operating in a market with specific local compliance requirements, or when you are scaling across multiple facilities with different configurations, custom development is often the more practical long-term investment.
The trade-off is clear: custom builds require a longer upfront investment in time, budget, and vendor selection. But they deliver systems that fit your operations rather than requiring your operations to fit the system.
What to look for in a custom HIS development partner
Not all software development firms have the depth to build healthcare systems. The risks of getting this wrong, including data breaches, compliance failures, and clinical workflow disruption, are significant. Look for:
Proven healthcare delivery track record. Ask for case studies with measurable outcomes, not just system screenshots. A vendor that has built and deployed HIS for hospitals similar to yours is a fundamentally different risk profile from one that is entering healthcare IT for the first time.
Compliance expertise built into the process. HL7 FHIR, HIPAA, GDPR, local MOH/DOH standards: these cannot be retrofitted at the end of a build. They need to be embedded in architecture decisions from day one. Ask how the vendor handles compliance in their standard development process.
Modular architecture. A custom HIS that cannot be extended without a full rebuild is not custom, it is just expensive. Modular design ensures you can add departments, integrate new tools, or expand to additional facilities without replacing the core system.
Post-launch support model. Healthcare systems do not get decommissioned after go-live. You need a vendor with a clear support model, SLAs, and the organizational stability to be a long-term partner.
9. Synodus

Synodus is a healthcare software development company with a team of over 250 developers, serving hospitals, aged care providers, and pharmaceutical companies across Vietnam, Australia, and the wider APAC region.
Their approach combines a packaged base system, covering core HIS modules like EMR, pharmacy, inventory, billing, and scheduling, with custom development for the workflows, integrations, and compliance requirements that are specific to each client. This hybrid model reduces time to deployment while preserving the flexibility that pure custom builds offer.
Their HIS case study for a Vietnamese university hospital documents a facility serving 5,000 outpatients and 1,700 medical staff daily, where the implementation delivered a 300% revenue increase, $70,000 in monthly administrative cost savings, 30% improvement in patient satisfaction, and a 0.01% insurance claim denial rate.
For a detailed breakdown of another implementation – Military Hospital 110, 70% efficiency boost in 4 months – see the hospital information system case study.
Best for: Mid-to-large hospitals in Asia-Pacific with complex workflows, local compliance requirements (Vietnam MOH, Australia TGA, Philippine DOH/PhilHealth), or multi-facility deployment needs that OTS products cannot serve well.
Projects start within 48 hours of scoping completion.
Head-to-head comparison table
| System | Best for | Deployment | Pricing range | Interoperability | KLAS / Review rating |
|---|---|---|---|---|---|
| Epic Systems | Large health systems, academic centers | Cloud / On-premise | $15M+ (enterprise) | HL7 FHIR, USCDI v3 | Industry-leading |
| Oracle Health | Large systems, government, VA | Cloud-native (OCI) | Enterprise pricing | HL7 FHIR, OCI-integrated | Recovering (KLAS 2024) |
| MEDITECH Expanse | Mid-size, community, rural | Cloud (MaaS) / On-premise | Custom quote | HL7 FHIR, Traverse Exchange | Top 2 (KLAS, 5 consecutive years) |
| Insta HMS | Mid-size, APAC/MENA | Cloud / On-premise | Affordable (custom quote) | HL7 | Positive user reviews |
| eClinicalWorks | Ambulatory, outpatient, US | Cloud | From $499/month | HL7 FHIR | Mixed (strong ambulatory) |
| Aarogya | Small-mid, South Asia | On-premise / Cloud | Affordable | Standard | Positive |
| eVisit | Small clinics, telehealth | Cloud | Higher-end for small practices | Standard | Positive, noted glitches |
| OpenMRS | NGO, public health, low-resource | Self-hosted / Cloud | Free (open-source) | HL7 FHIR | Strong in target markets |
| Synodus (custom) | Complex, APAC, multi-site | Custom | From $25/hr | HL7 FHIR, local standards | 5.0 (Clutch) |
Four questions to ask before you decide
Rather than starting with a vendor list, start with these four questions. The answers will tell you which category of system you actually need.
- What is your bed count and patient volume? Under 100 beds and relatively straightforward workflows: OTS cloud products like MEDITECH MaaS, eVisit, or Aarogya are worth evaluating first. Over 500 beds with multi-department complexity: the Epic/Oracle tier is where you should be looking, or a custom build if local compliance requirements rule out those vendors.
- What does your compliance landscape look like? US hospitals face HIPAA and USCDI interoperability requirements. European hospitals face GDPR plus national health IT standards. Asian hospitals face a patchwork of local MOH regulations, often with no clear English-language documentation. If your compliance environment is local and specific, verify that any vendor you evaluate has deployed successfully in that regulatory context before, not just in markets with similar-sounding regulations.
- What are you replacing, and how messy is the migration? Migrating from paper to digital is a different project from replacing one HIS with another. The latter involves data migration, staff retraining, and workflow redesign all at once. Your implementation timeline and budget should reflect this. See the hospital information system implementation plan for a phase-by-phase breakdown, and EHR implementation challenges for what typically goes wrong and how to avoid it.
- What is your 5-year plan? A system that fits today may not fit in three years if you are planning to add facilities, expand specialties, or scale patient volume significantly. Modular architecture and clear upgrade paths are not just nice to have: for any facility with growth plans, they are prerequisites.
For a deeper view of the vendor landscape including regional players, see the hospital information system companies guide. For a region-specific breakdown, the HIS providers in Malaysia guide and the Philippines HIS guide cover ASEAN markets in more detail.
FAQs
Epic Systems leads the global HIS/EHR market with approximately 42.3% of the US acute care hospital segment, followed by Oracle Health at 22.9% and MEDITECH at 14.8% (KLAS Research, 2025). Epic added a net 176 hospitals in 2024, its largest annual gain on record.
There is no single best HIS globally. Epic is the top-rated system for large health networks in North America and select international markets. MEDITECH Expanse leads for mid-size and community hospitals. For facilities in Asia-Pacific, MENA, or other regions with specific local compliance requirements, regional systems or custom-built platforms often deliver better fit than US-centric vendors. The right answer depends on your facility size, budget, compliance environment, and operational complexity.
No. Epic is the best choice for large health systems with the budget and IT capacity to support a complex, long-term implementation. For mid-size hospitals, MEDITECH Expanse consistently outperforms on cost and ease of use. For small or rural facilities, cloud-native products like eVisit or MEDITECH MaaS are more practical. For hospitals in emerging markets, regional or custom solutions often deliver better fit and compliance coverage than US-centric platforms.
An EHR (Electronic Health Record) is the clinical record layer: it stores patient data, diagnoses, medications, and treatment history. An HIS is broader: it integrates the EHR with administrative, financial, inventory, pharmacy, and operational systems across the entire hospital. In most modern implementations, the EHR is a module within the HIS rather than a standalone system. For a full breakdown, see EMR vs EHR vs PHR: what is the difference?
Small clinics deploying a cloud-based OTS system: 2-4 months. Mid-size hospitals: 6-12 months. Large health systems replacing legacy infrastructure: 12-24 months. Epic and Oracle implementations at large academic medical centers can run longer. Custom builds sit anywhere in the 6-18 month range depending on scope. For context, the MEDITECH MaaS model was specifically designed to compress implementation timelines for community hospitals.
It varies significantly by vendor and scope. Epic implementations for large systems run into the tens of millions. MEDITECH Expanse and mid-market OTS products use custom-quoted pricing based on bed count and modules selected. Open-source options like OpenMRS have no licensing fees but require technical implementation and maintenance investment. Custom development costs typically start around $50,000-$100,000 for smaller scope projects and scale into the hundreds of thousands for complex multi-department systems. For a detailed breakdown, see the hospital information system cost guide.
Critical. A system that cannot exchange data with your lab, imaging, pharmacy, and insurance billing systems creates the same information silos as paper-based records. At minimum, look for support for HL7 FHIR standards. In the US, USCDI v3 compliance is increasingly a procurement requirement. In other markets, check what the local health IT authority mandates. Poor interoperability is one of the most cited causes of failed HIS implementations. See types of healthcare software for an overview of how HIS connects with adjacent systems.
User adoption. A technically sound system that clinical staff resist using produces the same outcomes as no system at all. The most common causes of adoption failure are: inadequate training before go-live, failure to involve frontline staff in workflow design, and poor change management. Budget for change management as seriously as you budget for the software itself.
How useful was this post?
Click on a star to rate it!
Average rating / 5. Vote count:
No votes so far! Be the first to rate this post.




