How much does the hospital information system cost?
Let me be clear that these are just average numbers. Your hospital information system can be much lower or higher, depending on the development quality, project complexity and your requirements. Keep in mind that in addition to paying for the software, you also have to pay for development tools, maintenance fees, software updates and training fees.
There are two ways to acquire an HIS:
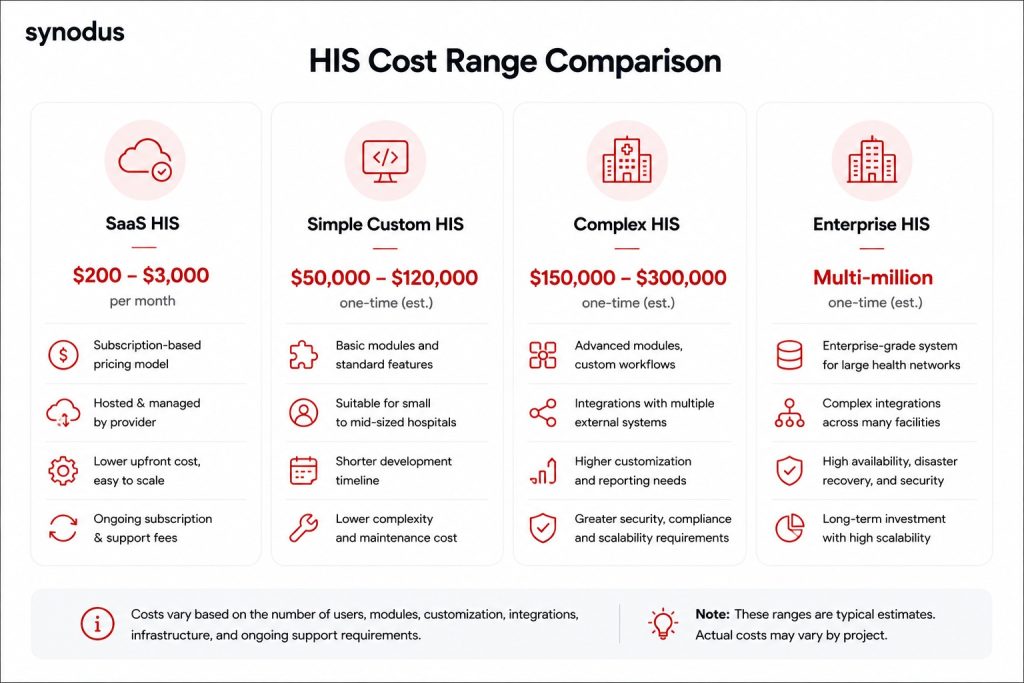
Custom development:
- Simple HIS (one platform): $50,000 to $120,000
- Complex system (cross-platform): $150,000 to $300,000
- Large hospital, multi-site: $300,000 to multi-millions
Off-the-shelf / SaaS subscription:
- Typical range: $200 to $3,000/month
- Fast to deploy, lower upfront cost, but limited flexibility and scalability
The sections below break down what drives these numbers so you can estimate your own project more accurately. For a side-by-side comparison of which system type fits your facility, see the top hospital information system guide.
Cost of off-the-shelf HIS packages
Off-the-shelf and SaaS HIS packages are priced per user or per module, typically on a monthly subscription model. The total cost of a package in a hospital information system depends on the number of users, modules selected, and deployment model.
Typical pricing tiers:
| Package type | Monthly cost | Best for |
|---|---|---|
| Basic (scheduling, billing, records) | $200 – $500/month | Small clinics, under 50 users |
| Mid-tier (full OPD/IPD, pharmacy, lab) | $500 – $1,500/month | Community hospitals, 50-200 users |
| Enterprise (full suite, multi-site) | $1,500 – $3,000+/month | Large facilities, 200+ users |
Hidden costs to budget for on top of subscription fees: onboarding and data migration ($5,000-$30,000 depending on data volume), staff training, and integration with existing lab or billing systems. Some vendors charge per API call for third-party connections – verify this before signing.
For a list of OTS vendors and what each is best suited for, see the hospital information system companies guide.
Cost factors for custom HIS development

Number of features
The more modules you include, the higher the cost. HIS modules fall into three categories:
| For doctors and staff | For administration | For patients |
|---|---|---|
| EMR/EHR, LIS, RIS, telehealth, e-prescription, appointment scheduling | Billing, insurance/claims, pharmacy management, HRM | mHealth/web portals, telemedicine, personal health reports |
Not all modules cost the same. Core modules like EMR/EHR, LIS, and RIS require extensive data processing, interoperability, and compliance work – making them significantly more expensive than simpler modules:
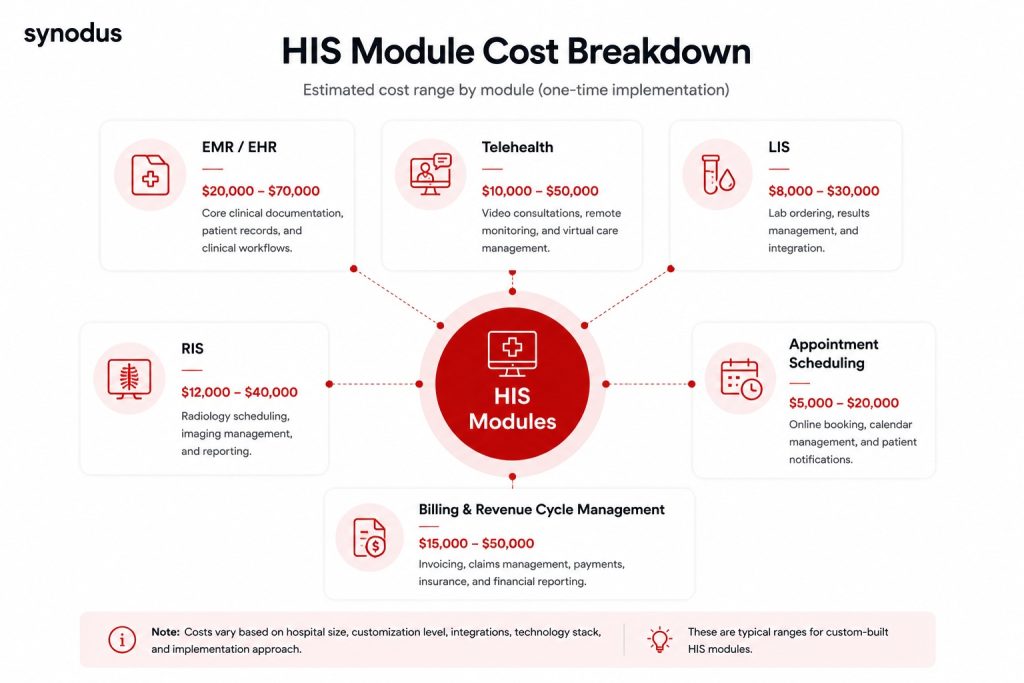
- Appointment scheduling: A few thousand dollars
- EMR/EHR module: $50,000 to $150,000 depending on customization and security requirements
- Telehealth and e-prescription: $30,000 to $100,000, due to real-time video, secure communication, and pharmacy integration
Adding advanced features inside modules – such as AI-powered decision support within EMR or predictive analytics in LIS – can increase costs by 20-40% but often generates higher ROI through efficiency gains.
Technology stack
The programming languages, frameworks, and databases you choose directly affect cost and long-term total cost of ownership (TCO).

- On-premises software (EHR/EMR, medical image analysis): $200,000 to $500,000, driven by hardware, infrastructure, and licensing
- Cloud-based HIS: $50,000 to $300,000 – eliminates heavy infrastructure investment, scales more predictably
- Mobile HIS applications: $50,000 to $200,000 for cross-platform with patient-facing features
- Web-based HIS: $20,000 to $100,000 – most cost-efficient for smaller hospitals or clinics
Advanced technology add-ons:
- AI/ML (diagnostics, predictive analytics): adds 20-40% to base cost
- Blockchain (record security, transactions): adds significant architecture complexity
- Big data analytics (population health, research): adds cost for data pipelines and visualization
Hidden costs often overlooked: system integration, data migration from legacy platforms, security compliance (HIPAA, GDPR), and ongoing DevOps typically add 15-30% on top of the base development cost.
Integration requirements
Every external system your HIS needs to connect with – existing hospital software, CRM, ERP, HRM, or third-party labs – adds cost. Standard API integrations are relatively affordable; older or custom-built hospital systems often require custom middleware or re-engineering, which can substantially raise the budget.
Budget specifically for compliance on data exchange. Sharing patient records between systems must meet HIPAA or GDPR requirements, which means spending on encryption, audit trails, and secure authentication. Plan for ongoing monitoring too – integrations can break when connected systems update their versions or data formats.
UI/UX design
HIS users range from senior surgeons to elderly patients. A system that clinical staff resist using produces the same outcome as no system at all, so UI/UX is not optional.
Budget for user research, usability testing, and iterative design cycles. Patient-facing portals need accessibility features: multilingual support, mobile-friendly layouts, and simplified navigation. Advanced features like data visualization dashboards or voice navigation improve usability but add design and development cost.
Testing and quality assurance
Healthcare software testing costs more than standard software testing because the stakes are higher. Testing should cover:
- Functional testing: Each module works correctly in isolation
- Integration testing: Data flows correctly between modules and external systems
- Performance and load testing: System handles peak concurrent users without degradation
- Security and compliance testing: Meets HIPAA, GDPR, HL7/FHIR standards
- User acceptance testing (UAT): Clinical staff can use the system accurately in real conditions
Security and performance testing typically account for 20-30% of total HIS development budget. This is not a place to cut costs – a compliance violation or data breach will cost far more than thorough testing upfront.
Development approach: In-house vs outsourcing
Outsourcing is almost always cheaper than building an in-house team for HIS development, primarily because it eliminates recruitment and HR overhead and gives access to a larger pool of specialists.
Typical hourly rates by region:
| Region | Hourly rate |
|---|---|
| Vietnam, India, Ukraine | $20 – $50/hr |
| Eastern Europe (Poland, Romania) | $40 – $80/hr |
| USA, Australia, Singapore, Western Europe | $80 – $200/hr |
Rate differences do not always reflect service quality. Many APAC vendors combine competitive pricing with strong healthcare IT experience – particularly in markets like Vietnam where HIS development for regional hospital networks is a mature practice.
When outsourcing, verify compliance handling directly. Ask for the vendor’s most recent security audit results and confirm their process for embedding HIPAA, GDPR, or local MOH compliance into architecture decisions, not just documentation at the end.
Team size
A larger team does not mean faster delivery. Research shows that a team of 30 developers produces fewer quality lines of code than a compact team of 4. More developers mean more coordination overhead, more meetings, and more integration issues.
The optimal structure for most HIS projects:
- Core team (5-10 people): Backend, frontend, database, QA
- Extended specialists (as needed): Compliance, data analytics, AI, integration
- Management layer: Scrum Master, Product Owner running Agile cycles
Outsourcing vendors typically offer flexible team scaling – starting small and adding members as the project scope expands is both cost-efficient and quality-preserving.
Hardware costs
For on-premises deployments, hardware is a significant cost line:
- Small clinics: Basic servers and networking – a few thousand to tens of thousands of dollars
- Large hospitals or multi-site systems: High-capacity servers, redundant storage, disaster recovery – easily into the hundreds of thousands
Cloud-based deployments eliminate most hardware costs. Specialized medical devices connected to HIS (imaging machines, bedside monitors, IoT equipment) may still require integration gateways regardless of deployment model.
Example cost breakdown: Custom HIS with Synodus
A typical Synodus HIS project runs 5-7 people at $25-$35/hour:
- 1 project manager
- 1-2 testers / QA
- 2-4 developers
- 1 UX/UI designer
Project phases and estimated effort:
| Phase | Small project | Mid-size project | Large project |
|---|---|---|---|
| Product discovery | Free (scoping session) | Free (scoping session) | Free (scoping session) |
| Architecture + UX/UI design | 25-60 hours | 60-120 hours | 150+ hours |
| Development | 2-3 months | 3-6 months | 6-12+ months |
| Testing | A few days | 1-2 weeks | 2-4 weeks |
Estimated total cost by project size:
| Project size | Scope | Estimated cost |
|---|---|---|
| Small | Single-platform, core modules only | $50,000 – $120,000 |
| Mid-size | Cross-platform, full module set | $150,000 – $300,000 |
| Large | Multi-site, advanced integrations, AI | $300,000+ |
The key to keeping costs predictable at Synodus is the packaged solution approach: rather than building from scratch, they start from a pre-built HIS architecture and customize it to your requirements. This skips the foundation-building phase and compresses timelines significantly.
For real examples of how this plays out in production, see the HIS case study.
Tips to reduce hospital information system cost
Based on working with 30+ healthcare facilities and 10,000+ healthcare staff:
- Outsource to a lower-cost region (Vietnam, India, Ukraine) for the same technical quality at 40-60% lower rates than US or Australian vendors
- Choose the right cooperation model: Staff augmentation for filling a specific in-house role; project-based for a full build without an internal team
- Start with core modules and add complexity in phases – avoids overbuilding upfront and spreads cost over time
- Use agile methodology for faster iteration and early bug detection
- Leverage a packaged base system rather than building from scratch – the biggest single driver of cost and timeline reduction
- Sign an SLA with clear penalties for missed deadlines and quality benchmarks
At Synodus, healthcare domain expertise, compliance knowledge, and competitive pricing come as a package. Projects start within 48 hours of scoping completion.
Wrapping up
Hospital information system cost is not just the software purchase price. The base development or licensing fee is typically only half the story. Hidden costs that commonly catch hospitals off guard:
- Integration work: Each legacy system your HIS connects to (lab analyzers, imaging systems, insurance portals) adds custom development scope that initial quotes rarely capture accurately
- Compliance updates: Regulatory changes (new HL7 versions, updated PhilHealth eClaims standards, MOH mandate changes) require ongoing development work, not a one-time fee
- Data migration: Cleaning and migrating years of paper or legacy digital records is consistently underestimated in both time and cost
- Training and change management: Staff training across multiple departments, plus the productivity dip during the transition period, are real costs that do not appear in vendor quotes
- Post-go-live support: The first 3-6 months after launch typically require intensive vendor support that is either included at a premium or billed separately
Breaking down costs by factor before you engage vendors gives you a realistic budget and stronger negotiating position. A vendor who cannot itemize these categories in their proposal is telling you something.
For the next step – comparing specific vendors by cost tier and hospital type – see the best hospital information system guide and the hospital information system companies guide.
FAQs
The cost of EMR/EHR systems depends on deployment type, number of users, and features.
– SaaS EMR/EHR: $600 to $1200 per year per user.
– Custom EMR/EHR development: $50,000 to $150,000 upfront cost. Some projects can cost more than $150K with a complex scope.
You can find more details here.
ROI shows up in reduced administrative workload, faster patient turnover, fewer diagnostic errors, improved billing accuracy, and patient satisfaction scores. Most hospitals start seeing measurable ROI 18-24 months after implementation when cost optimization strategies are applied from the start. For a breakdown of the implementation phases that drive these outcomes and when to expect them, see the hospital information system implementation guide.
For a stakeholder-by-stakeholder breakdown of what ROI actually looks like with real data, see hospital information system benefits: what the data shows.
Licensing fees for third-party integrations, regulatory compliance updates, cybersecurity measures, staff training, hardware upgrades, and post-deployment support. Integration costs are particularly easy to underestimate – each legacy system your HIS needs to connect with adds scope that is rarely captured accurately in initial quotes.
Choosing a modern stack (cloud-native, microservices, open-source frameworks) lowers licensing and maintenance cost. Legacy stacks or proprietary solutions may raise initial integration expenses and lock hospitals into costly vendor dependencies.
Yes. Agile allows iterative module delivery and early user feedback, reducing the risk of developing unused or outdated features. Waterfall often inflates cost due to large upfront planning and expensive reworks when requirements shift.
How useful was this post?
Click on a star to rate it!
Average rating / 5. Vote count:
No votes so far! Be the first to rate this post.




