What is the hospital information system?
Hospital Information System (HIS) – also called Hospital Management System (HMS), Hospital Management Information System (HMIS), or Hospital Information Management System (HIMS) – is a comprehensive, integrated healthcare software platform that centralizes clinical, administrative, and financial data across a hospital.
Unlike standalone tools such as Electronic Medical Records (EMR) or Electronic Health Records (EHR), an HIS connects every department into a unified ecosystem covering patient management, clinical documentation, scheduling, inventory, billing, and regulatory compliance.
Today, leading hospitals adopt HIS not only to store patient data, but also to:
- Automate time-consuming workflows (scheduling, billing, inventory tracking)
- Ensure interoperability between departments and external systems
- Enhance patient safety through real-time alerts and complete medical histories
- Support digital health transformation and compliance with regulations like HIPAA, HL7, and GDPR
In short, HIS acts as the central nervous system of modern hospital IT infrastructure – one source of truth that every department draws from.
History of hospital information systems
Understanding where HIS came from helps explain why modern systems are designed the way they are.
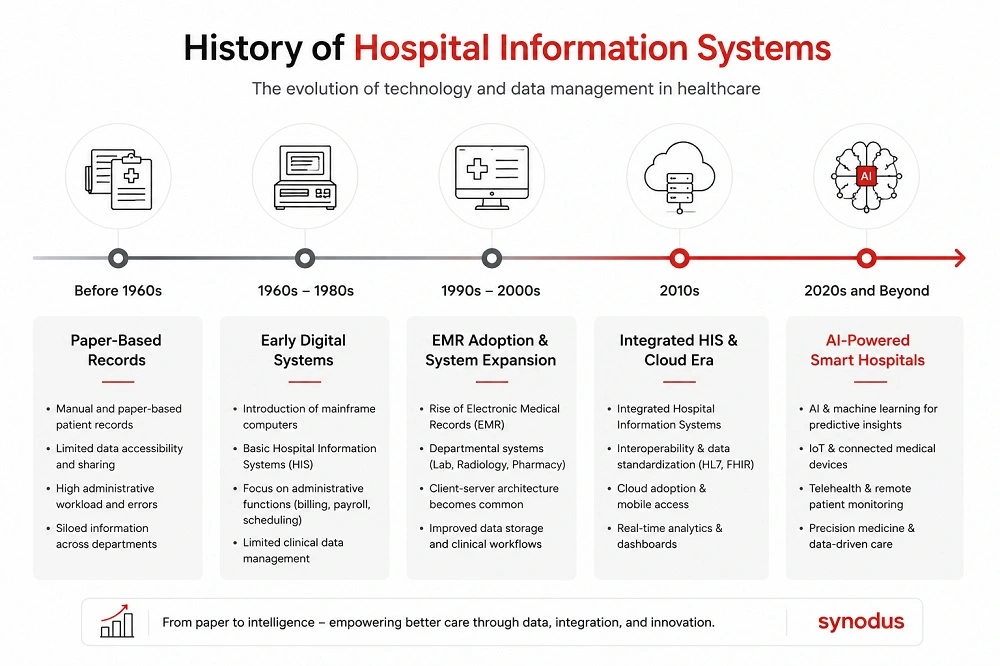
1960s – 1970s: The beginning of digitalization
Early HIS focused on administrative tasks – billing, payroll, and inventory – running on mainframe computers. They were expensive, limited in scope, and only accessible to large hospitals.
1980s: Expanding into clinical functions
With the rise of personal computing, hospitals began digitizing clinical departments: laboratories, radiology, and pharmacies. This was the first step toward hospital-wide data management.
1990s: Integration and connectivity
Local networks allowed departmental systems to share data. EMR systems emerged, laying the groundwork for today’s EHRs, making patient data more accessible and consistent across departments.
2000s: Digital transformation era
Global healthcare reforms and compliance standards drove wider HIS adoption. Systems evolved into web-based platforms supporting interoperability and clinical decision support.
2010s – present: Cloud, AI, and connected healthcare
Modern HIS are cloud-based, mobile-enabled, and powered by AI, IoT, and advanced analytics. They don’t just store data – they help hospitals predict risks, optimize resources, and deliver value-based care.
The global hospital information system market reflects this shift. According to MarketsandMarkets, the market was valued at $58.13 billion in 2023 and is projected to reach $116.75 billion by 2030, growing at a CAGR of 10.6%. Key drivers include mandates for electronic records, rising hospital digitalization in Asia-Pacific and the Middle East, and growing demand for interoperability between care settings.
Types and classification of HIS
HIS can be classified by function, architecture, or scope. Understanding these helps healthcare organizations select the right system for their needs.
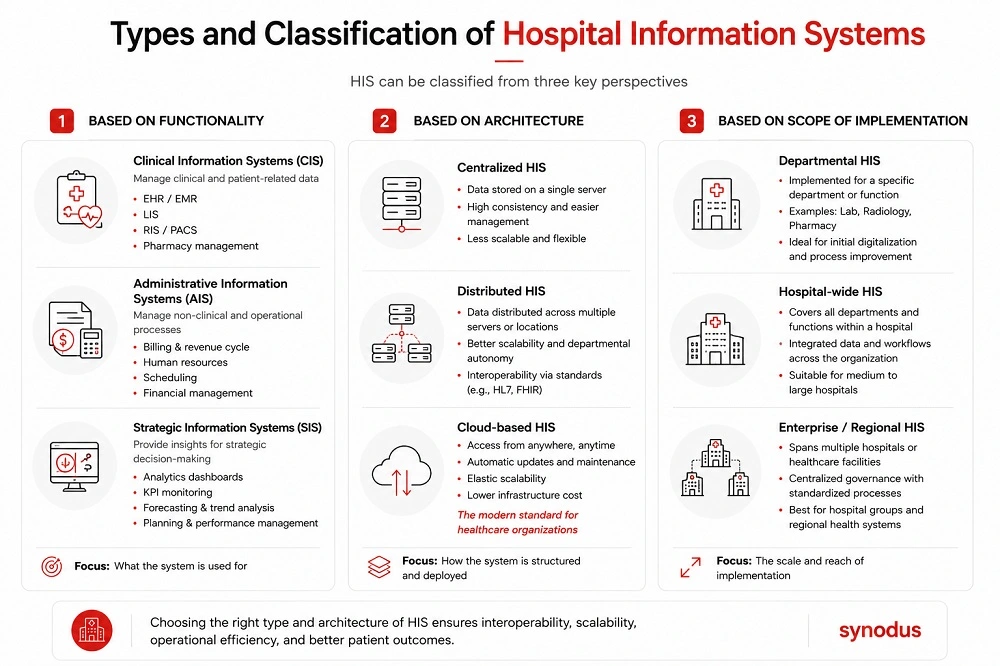
Based on functionality
Clinical Information Systems (CIS) manage patient-facing clinical data: EHR/EMR, laboratory results (LIS), radiology imaging (RIS/PACS), and pharmacy management. They support clinical decision-making and patient safety.
Administrative Information Systems (AIS) handle non-clinical operations: billing, human resources, scheduling, and financial management. They keep the business side of a hospital running efficiently.
Strategic Information Systems (SIS) serve hospital executives with analytics dashboards, performance indicators, and forecasting tools to support long-term planning.
By architecture
Centralized HIS stores all data on a single server. High consistency, easier management, but less flexible at scale.
Distributed HIS spreads data across multiple servers or locations – better for scalability and departmental autonomy while maintaining interoperability through standards like HL7 or FHIR.
Cloud-based HIS is the modern standard: remote access, automatic updates, elastic scalability, and lower upfront infrastructure cost. Ideal for growing healthcare organizations.
Based on scope of implementation
| Scope | Description | Best for |
|---|---|---|
| Departmental HIS | Serves a single unit (lab, radiology, pharmacy) | First-step digitalization |
| Hospital-wide HIS | Integrates all departments into one platform | Mid-to-large hospitals |
| Enterprise / Regional HIS | Spans multiple facilities or a healthcare network | Hospital groups, regional health systems |
HIS vs Health Information System: The term “Health Information System” (HIS) is also used at the national or public health level – by WHO and ministries of health – to describe systems that aggregate population-level data for policy and planning. Hospital Information System refers specifically to the operational software running within a single hospital or hospital network. The acronym overlaps; the scope does not.
Key benefits of HIS
The business case for HIS is well-documented. Here are the core benefits, backed by peer-reviewed research:

1. Improved patient care and safety
HIS gives clinicians instant access to complete, up-to-date patient records – medication history, allergies, lab results, imaging – at the point of care. This directly reduces diagnostic errors and adverse drug events.
The evidence is substantial. A 2023 study published in npj Digital Medicine (Nature) tracked a hospital’s transition from paper-based to fully digital records and found a 38% reduction in voluntarily reported medication incidents post-transition, with prescribing errors dropping from 52.8% to 15.7% of orders reviewed. A separate systematic review and meta-analysis published in JAMIA found that computerized order entry systems were associated with roughly half as many preventable adverse drug events compared to paper-based order entry (pooled risk ratio of 0.47).
2. Operational efficiency and paperless workflows
HIS eliminates the bottlenecks of manual, paper-based processes. Nurses spend less time on documentation; administrative staff automate billing and scheduling; managers get real-time dashboards instead of waiting for end-of-day reports.
Research on hospital efficiency improvement programs – including digitalization – found cost reductions of 25-50% achievable through systematic digital and process interventions, allowing hospitals to reallocate resources toward direct patient care. Administrative expenses already represent 15-30% of total US hospital spending, making this one of the highest-impact areas for digitalization to address.
3. Regulatory compliance and data security
HIS provides a centralized, standardized, and auditable way of storing hospital data – making compliance with HIPAA, GDPR, HL7, and local healthcare regulations significantly easier. Role-based access control, audit logs, and encryption protect sensitive patient data from breaches.
4. Cost savings and resource optimization
HIS reduces expenses on printing, physical storage, and redundant administrative staffing. Automated processes prevent costly billing errors and claim rejections. Inventory management modules prevent both costly overstocking and dangerous medicine shortages.
On ROI, a study published in Health Affairs found that medical practices recovered their EHR investment costs within 2.5 years on average, with each full-time staff member generating over $20,000 in additional net revenue annually post-implementation – primarily through improved coding accuracy and productivity. For medication management automation specifically, a European analysis covering EU27 + UK hospitals modeled an average payback period of 4.46 years with an average ROI of 167% over a 10-year horizon.
5. Better financial visibility
Integrated billing, insurance claims processing, and financial reporting give hospital administrators a real-time view of revenue cycles. This reduces claim denials, accelerates reimbursements, and improves cash flow predictability.
For a deeper breakdown of each benefit backed by research data, see benefits and advantages of hospital information system.
Core modules of HIS
An HIS is not a single piece of software, it is a system of interconnected modules. The exact combination depends on your facility’s size, type, and operational needs.
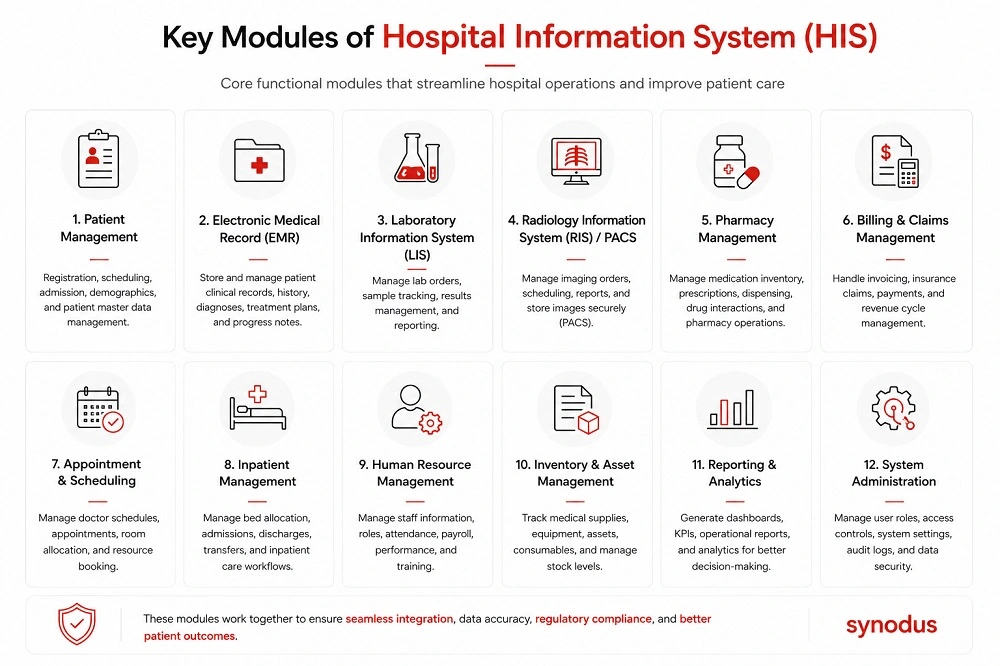
1. Core system (Patient data management / EHR)
The foundation of any HIS. This module manages every patient’s digital record – demographics, medical history, diagnoses, medications, and treatment plans. It is often built around or integrated with an EHR/EMR system and supports administrative tasks like appointment scheduling and patient assignment.
2. Business and financial system
Manages financial operations: billing, insurance claims, healthcare accounting, and reimbursement tracking. Automation here reduces human error and accelerates the revenue cycle. Reporting tools give finance teams and hospital administrators visibility into the facility’s financial health.
3. Departmental management system
Each clinical department may have a dedicated sub-system, all connected to the central HIS:
- LIS (Laboratory Information System): Manages test orders, results, and lab workflow
- RIS (Radiology Information System) + PACS: Stores and transmits medical images (X-rays, MRI, CT scans)
- Pharmacy Management System: Tracks prescriptions, drug inventory, and dispensing
- Patient Tracking System: Supports remote patient monitoring and telehealth integration

4. Inventory and procurement system (PIMS)
Tracks supply chain and usage of medicines, chemicals, and medical equipment. Alerts staff when stock runs low. Integrates with procurement to automate purchase orders. This module is especially critical for large hospitals managing thousands of SKUs across multiple wards.
5. Human resources management system (HRM)
Manages staff records, scheduling, payroll, performance tracking, and training compliance. While some hospitals keep this separate from HIS, integrating HR data with clinical scheduling significantly improves workforce planning and reduces coverage gaps.
Must-have features of hospital information system
Not all HIS implementations include every module above, but these features are essential for any system to deliver real value:
Patient management: A comprehensive view of each patient’s journey: personal information, medical history, diagnoses, medications, and treatment plans. Supports continuity of care across departments and visits.
Appointment scheduling: Online and in-person scheduling that reduces wait times, prevents double-bookings, and helps administrators assign doctors and rooms more accurately. Good scheduling systems also send automated reminders to reduce no-shows.
Billing and financial management: Automated payment processing, insurance claim submission, and reimbursement tracking. Minimizes human error and speeds up the revenue cycle.
Pharmacy and inventory management: Tracks medication dispensing, monitors stock levels, and flags potential drug interactions or shortages before they become crises.
Electronic prescriptions and clinical alerts: Doctors issue digital prescriptions instantly. The system checks for drug interactions, allergies, and dosage issues in real time, preventing errors before they reach the patient.
Communication and reporting: Real-time messaging between departments, performance dashboards for managers, and compliance reporting for regulators. Reduces information silos and improves cross-department coordination.

Real-world use cases

Public hospitals: Managing high patient volumes
Large government-funded hospitals deal with thousands of patients daily. HIS helps manage bed occupancy in real time, automate high-volume billing, and maintain compliance with strict regulatory standards. Without it, the administrative load becomes unmanageable at scale.
Private hospitals and clinics: Competing on patient experience
Private healthcare providers compete by delivering superior, personalized care. HIS-powered appointment scheduling, patient tracking, and billing integration reduce wait times and improve satisfaction scores. Analytics dashboards help private hospitals make smarter operational decisions.
Specialty centers (oncology, cardiology, etc.)
Long-term treatment for complex conditions requires coordinating across multiple specialists, tracking treatment cycles over months or years, and maintaining detailed clinical records. HIS enables centralized treatment records, lab/radiology integration, and secure data sharing across multidisciplinary care teams.
Telehealth and remote care
Post-pandemic healthcare has shifted significantly toward digital delivery. Modern HIS platforms integrate with telemedicine tools to support online consultations, e-prescriptions, and remote patient monitoring – allowing hospitals to extend care beyond physical walls.
Academic and research hospitals
University hospitals need reliable, de-identified patient data for clinical trials, research studies, and training programs. HIS facilitates secure data collection, reporting, and export in formats required by research institutions and ethics committees.
Synodus’ case examples
Vietnam University hospital: Full-facility digitalization
One of Vietnam’s leading university hospitals – serving 5,000 outpatients daily with 1,700 medical staff – was relying heavily on paper-based processes and disconnected departmental systems. Getting a complete picture of any patient required staff to cross-reference multiple records manually, adding friction to every clinical decision.
Synodus built a full HIS covering integrated EMR, inventory management, quality analytics dashboard, and a patient-facing mobile app for appointment scheduling, test result access, and online consultations. The system was built to comply with Vietnam MOH regulations and designed around the hospital’s specific operational model.
Results after deployment:
- 300% revenue increase
- $70,000/month in administrative cost savings
- 30% improvement in patient satisfaction
- 10 new specialized faculties established
- 50% of appointments pre-booked via mobile and web app
- 0.01% insurance claim denial rate
Military Hospital 110: Mid-size digitalization in 4 months
Military Hospital 110 serves 1,500 outpatients and 500 inpatients daily with 500 healthcare staff. Despite its scale, the facility was receiving consistent complaints about slow response times and lost patient data across departments. Staff spent more time managing paperwork than treating patients.
Synodus built a custom HIS in 4 months using a packaged base extended with custom modules: EMR connected via IoT to LIS and PACS, automated scheduling and bed management, billing and inventory, a bilingual patient mobile app, and a training coordination module. Full compliance with Vietnamese data protection law, HL7, ISO, and HIPAA standards.
Results after deployment:
- 70% boost in operational efficiency
- 85% of reports and forms digitalized
- 90% decrease in incidents: late responses, disparate data, wrong diagnoses
- Under 2 minutes average sync time for patient records across departments
- 100% adoption across all departments and staff
Build your HIS with Synodus
Synodus is a Vietnam-based healthcare software development company with 250+ developers, 30+ healthcare clients across APAC, and a 5.0 rating on Clutch.
Their hybrid model starts from a validated HIS base covering EMR, pharmacy, inventory, billing, and scheduling, then builds custom workflows, integrations, and compliance layers around each client’s specific context. This approach reduces time-to-go-live while preserving the flexibility that off-the-shelf products cannot offer.
Services include:
- Custom HIS development – built around your workflows, local compliance (MOH, DOH, PhilHealth, HIPAA, HL7, FHIR), and integration needs
- EMR/EHR development – clinical record systems with full audit trails and regulatory compliance
- Patient mobile apps – bilingual, mobile-first interfaces for scheduling, teleconsultation, and record access
- LIS, RIS, PACS integration – IoT-connected laboratory and imaging systems feeding into a centralized EMR
- Inventory and pharmacy management – real-time supply tracking, dispensing alerts, and procurement automation
- Analytics dashboards – operational and clinical performance visibility for hospital management
Projects start within 48 hours of scoping completion.
How to choose the right HIS
Healthcare providers generally have three main options when acquiring an HIS:
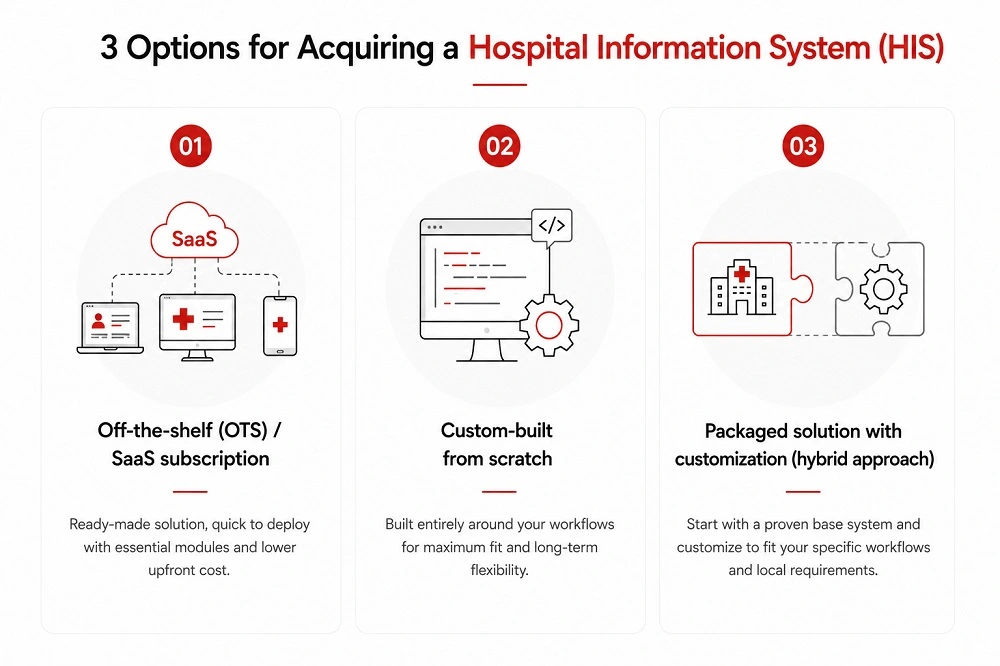
Option 1: Off-the-shelf (OTS) / SaaS subscription Ready-made solutions are fast to deploy and cost-effective upfront. They cover essential modules (patient management, billing, pharmacy) and require minimal IT investment. The trade-off is limited customization, potential vendor lock-in, and may not align with your specific workflows or local compliance requirements.
OTS HIS pricing typically ranges from $200 to $3,000/month for SaaS subscriptions, depending on the number of users and features.
Option 2: Custom-built from scratch A system built entirely around your facility’s workflows ensures maximum fit and long-term flexibility. It requires a higher upfront investment in time, budget, and technical expertise – typically $50,000 to $300,000+ depending on complexity – but delivers the strongest long-term ROI for facilities with unique or complex needs.
Option 3: Packaged solution with customization (hybrid approach) Start with a pre-built base system that covers all the fundamentals, then customize and extend it to fit your specific workflows and local requirements. This balances cost-efficiency with adaptability and is increasingly the preferred approach for mid-to-large hospitals.
Reference: Popular OTS HIS software:
| Software | Primary strength |
|---|---|
| Aarogya | Pharmacy management |
| eHospital | Patient data management and performance analytics |
| eVisit | Patient self-service portal and e-prescribing |
| myNapier | Healthcare billing and insurance claims |
| Insta HMS | Outpatient management |
| ProMed | Inpatient management |
| Epic | Enterprise-scale EHR and HIS integration |
If you’re looking for a side-by-side comparison of the leading options on the market, see our guide to the best hospital information systems available today.
Key criteria to select the right HIS
When evaluating HIS vendors, these are the criteria that matter most:

Scalability – Healthcare is a high-growth, high-change environment. Your HIS must be able to add modules, handle more users, and expand to new facilities without requiring a full system replacement. Extensibility is not optional.
Interoperability – Does the system support HL7, FHIR, or DICOM standards? Can it integrate with your existing lab, radiology, or billing systems? Poor interoperability is one of the most common causes of HIS failure.
Ease of use – HIS users include doctors, nurses, administrative staff, and patients of all ages and technical backgrounds. A system that’s difficult to use will be resisted, resulting in parallel paper processes and negating the benefits of digitalization.
Compliance and localization – The system must support local regulatory requirements (HIPAA in the US, PDPA in Thailand, MOH standards in Vietnam, etc.), local languages, and local billing and insurance workflows.
Vendor experience in healthcare – Healthcare IT is a specialized domain. The vendor needs to understand not just software development, but clinical workflows, data privacy requirements, and the operational realities of running a hospital.

Common challenges and how to solve them
Off-the-shelf limitations
The problem: Standardized HIS products can’t accommodate the unique workflows, compliance requirements, and departmental structures of every hospital. What works for a 50-bed private clinic may not work for a 500-bed public teaching hospital.
The impact: Workarounds accumulate. Staff maintain shadow paper processes. Small operational changes – new regulations, new treatment protocols, staff expansion – may require a full system replacement.
The solution: Plan for customization from the start. If a pure custom build is too expensive initially, a packaged solution with modular add-ons offers the best balance of speed and long-term flexibility. Involve end users (doctors, nurses, administrators) in requirements definition – not just IT or management.
Data privacy & security
The problem: Digitizing hospital operations means storing vast amounts of sensitive patient data on interconnected systems. This creates exposure to data breaches, ransomware attacks, and compliance violations.
The impact: A single security incident can result in significant financial penalties (up to millions of dollars under HIPAA or GDPR), reputational damage, and loss of patient trust that takes years to rebuild.
The solution: Require vendors to implement end-to-end encryption, multi-factor authentication, role-based access control, and regular penetration testing. Compliance with relevant standards (HIPAA, GDPR, ISO 27001) should be demonstrated – not just claimed.
User adoption resistance
The problem: Not all clinical staff are tech-savvy, and many perceive new systems as an additional burden rather than a tool. Resistance is especially common among senior clinicians who have decades of established routines.
The impact: Low adoption slows workflows, undermines the benefits of the investment, and often results in dual systems running in parallel – digital and paper – which increases workload rather than reducing it.
The solution: Invest in a user-centric design process where clinical staff have input on interface decisions. Plan a proper change management program: training, superuser networks, a phased rollout, and clear channels for feedback and issue reporting. Adoption doesn’t happen on go-live day – it’s a process that requires ongoing support.
Wrapping up
A Hospital Information System is not just software – it’s the operational infrastructure that determines whether a healthcare facility can function efficiently, safely, and sustainably at scale.
The right HIS improves patient outcomes, reduces administrative burden, strengthens regulatory compliance, and provides the data visibility that hospital leaders need to make good decisions. Getting there requires careful planning: choosing the right modules, the right architecture, and the right implementation partner.
Whether you’re evaluating an off-the-shelf system, building custom, or somewhere in between – the key is to start with a clear picture of your operational needs, your compliance requirements, and your growth trajectory.
FAQs
HIS serves multiple user groups: doctors and nurses (clinical modules), administrative staff (billing, scheduling), IT teams (system management), hospital managers (analytics and reporting), and patients (self-service portals and mobile apps).
An EMR (Electronic Medical Record) is a digital version of a patient’s chart – it stores clinical data for use within a single facility. An HIS is broader: it integrates EMR with administrative, financial, and operational systems across the entire hospital. The EMR is a component of the HIS, not a replacement for it.
Both share the same acronym but operate at different levels. Health Information System (also HIS) is used by WHO and national health ministries to describe population-level data systems for public health planning. Hospital Information System refers to the operational software running within a hospital or hospital network.
Yes, but integration quality depends heavily on whether the HIS supports standard interoperability protocols like HL7 FHIR or DICOM. Before committing to a vendor, verify their integration track record with your specific existing systems and ask for references from similar implementations.
Not always. Off-the-shelf solutions offer fast deployment and lower upfront costs – they’re a strong fit for smaller facilities or those with standard workflows. Custom HIS provides the flexibility needed for complex, high-volume, or specialty facilities. Many hospitals now favor a hybrid approach: a standardized base system customized for their specific needs.
Aligning the system with the hospital’s unique operational workflows is consistently the biggest challenge. This requires thorough requirements gathering with all stakeholder groups before development begins – not just IT or hospital management, but the doctors and nurses who will use the system daily.
Choose vendors that implement encryption at rest and in transit, multi-factor authentication, role-based access control, and regular security audits. Ensure the system complies with applicable regulations (HIPAA, GDPR, or local equivalents). Conduct penetration testing before go-live and establish an ongoing security review cadence.
HIS supports nursing administration through improved care coordination, automated workflow management, and better decision support. Nurses can access complete patient records, update care plans in real time, communicate directly with physicians through the system, and receive automated alerts for critical patient changes – without leaving the bedside or hunting through paper files.
A Healthcare ERP focuses primarily on back-office functions: finance, HR, supply chain, and procurement. An HIS covers both clinical and administrative functions. Some modern platforms blur this distinction, but in most implementations, ERP and HIS serve complementary rather than overlapping roles. Read more on healthcare ERP here.
How useful was this post?
Click on a star to rate it!
Average rating / 5. Vote count:
No votes so far! Be the first to rate this post.




